The Body Fluids Are Multi-Dimensional – The Sea of L.I.F.E. – Living Interstitial Fluid Environment
There are 2 body fluids in the human body: Intracellular [1], Extracellular fluids.[2]Intracellular fluids are the fluids inside of a body cell.[3] Extracellular fluids have two types of fluids: intravascular fluids which are the fluids inside of the blood vessels.
This fluid is also called blood plasma.[4] The second type of body fluid is interstitial fluids of the Interstitium organ which are the fluids held in compartments found between blood vessels of all body cells which make up the body organs, glands and tissues. [5] In addition there are accumulation of interstitial fluids in compartments which have specific names and generally are referred to as transcellular fluids. These interstitial fluids include : lymphatic fluids, synovial fluids, pericardial fluids, cerebrospinal fluids, peritoneal fluids, pleural fluids, intraocular fluids, urinary lumen fluids and G.I.lumen fluids.[6][7][8]
Distribution of blood plasma, intracellular fluids, interstitial fluid and lymphatic fluid in human body has an embedded multi-dimensional network of blood and lymphatic capillaries along with interstitial fluid compartments called the Interstitium organ containing significant amounts of abundant blood-derived proteins, metabolic and dietary acids, fats, sodium bicarbonate and glucose.[9]

[Figure 1 – Multi-dimensional distribution of blood (intravascular fluids), Interstitium (interstitial fluids), body cells (intracellular fluids), lymph (interstitial fluids eliminated through the lymphatic circulatory system) and transcellular (interstitial fluids deposited in body cavities outside the Interstitium) make up the sea of life.[10]
Body Fluid Shifts
Body fluid shifts occur when the body’s fluids move between the three fluid compartments, the blood, the interstitial fluids or the Interstitium compartments and the intracellular fluids.

Physiologically, this occurs by a combination of hydrostatic pressure gradients and osmotic pressure gradients. Water will move from one space into the next passively across a semi-permeable membrane until the hydrostatic and osmotic pressure gradients balance each other. Many health conditions can cause body fluid shifts. When body fluids move out of the vascular compartments (the blood vessels), blood pressure can drop to dangerously low levels, endangering critical organs such as the brain, heart and kidneys; when it shifts out of the body cells or intracellular fluid compartments, cellular processes slow down or increase intracellular dehydration; when excessive fluid accumulates in the interstitial space, oedema develops; and fluid shifts within the interstitial fluids of the brain, this can cause increased cranial pressure or headaches, even migraine headaches. Body fluid shifts can be compensated with increased alkaline fluid replacement, increased alkaline mineral salts, improved blood, improved interstitial and lymphatic circulation and opening up the channels of elimination which include, urination, defecation, respiration and perspiration. The process of increased body fluid replacement, increased alkaline mineral salts, improved body fluid circulation and opening up the channels of elimination.
Third Body Fluid Spacing
“Third spacing” is the abnormal accumulation of fluids into the interstitial fluids of the Interstitium compartments and other interstitial fluids referred to as the transcellular space. In medicine, the term is often used with regard to loss of fluids into interstitial spaces of the Interstitium, such as with burns or edema, but it can also refer to body fluid shifts into a body cavity (transcellular space), such as with ascites and pleural effusions. With regard to severe burns, fluids may pool on the burn site (i.e. fluid lying outside of the interstitial fluid compartments of the Interstitium, exposed to evaporation) and cause depletion of the fluids. With pancreatitis or ileus, fluids may “leak out” into the peritoneal cavity, also causing depletion of the intracellular, interstitial or vascular compartments.Patients who undergo long, difficult operations in large surgical fields can collect third space body fluids and become intravascularly depleted despite large volumes of intravenous electrolyte fluid replacement by intravenous infusions or IV’s.[11]
The precise volume of fluid in the third spaces changes over time and is difficult to accurately quantify.Third body fluid retention conditions may include peritonitis, pyometritis, and pleural effusions.[12] Hydrocephalus and glaucoma are theoretically forms of third spacing, but the volumes are too small to induce significant shifts in blood volumes, or overall body fluid volumes, and thus are generally not referred to as third body fluid spacing.
The Multi-Dimensional Flow of All Body Fluids
All body cells that make up all organs, glands and tissues are continuously bathed in interstitial fluids of the Interstitium. The interstitial fluids are formed by leakage of blood plasma through minute pores of the capillaries. There is a continual interchange of fluid from the blood plasma and the interstitial fluids contained in compartments of the Interstitium with a free interchange of nutrients and other dissolved substances. Most of the interstitial fluids return to the circulatory system by means of capillaries or capillary pools, which feed into larger veins. Large protein molecules that have escaped from the arterial capillaries cannot reenter the blood circulation through the small pores of the capillaries. However, these large molecules, as well as white blood cells, dead cells, bacterial debris, acidic dietary and metabolic waste, larger particulate matter from cellular breakdown, and pleomorphic matter such as bacteria, yeast and mold can pass through the larger pores of the lymphatic capillaries and, thus, enter the lymphatic circulatory system with the remainder of the interstitial fluids of the Interstitium organ.
The Lymphatic System
The lymphatic system is the main circulatory system for removing acidic dietary, metabolic, respiratory and cellular waste from the compartments of the Interstitium containing interstitial fluids thus maintaining the alkaline design of all body fluids at 7.365, including the blood plasma, intracellular fluids and transcellular fluids. The activities of the Interstitium organ is supported by white blood cells called lymphocytes, which release alkaline chemical compounds to buffer or neutralize dietary and metabolic acids, such as lactic acid, citric acid, uric acid, nitric acid, carbon dioxide, glucose, which are all disease-causing agents.

[Figure 2 – Circulation of Interstitial fluids of the Interstitium organ compartments containing intravascular and intracellular fluids flow into the lymphatic capillaries for the purpose of eliminating toxic acidic metabolic waste through the pores of the skin or returned back to blood via the lymphatic system to be eliminated via the lungs, bowels or kidney’s.] [13]
Pathways of the Lymphatic Circulatory System
The lymphatic circulatory system pathways begin with lymphatic capillaries. These small tubes merge to form lymphatic vessels, and the lymphatic vessels in turn lead to larger vessels that join with the veins of the vascular system in the thorax.
Lymphatic Capillaries
Lymphatic capillaries are closed-ended tubes of microscopic size (Figure 2). They extend into interstitial fluids of the Interstitium compartments, forming complex networks that parallel blood capillary networks. The lymphatic capillary wall consists of a single layer of squamous epithelial cells. This thin wall makes it possible for interstitial fluid to enter the lymphatic capillary. Once the interstitial fluid from the Interstitium compartments enters the lymphatic capillaries, the interstitial fluid is called lymphatic fluid.
Lymphatic Vessels
Lymphatic vessels are formed from the merging of lymphatic capillaries. Lymphatic vessels, also known simply as lymphatics, are similar to veins in structure. The vessel walls are composed of three layers: an inner layer of endothelial tissue, a middle layer of smooth muscle and elastic fibers, and an outer layer of connective tissue.Like a vein, the lymphatic vessel has valves to prevent backflow of lymphatic fluids. The larger lymphatic vessels lead to specialized organs called lymph nodes. After leaving these structures, the vessels merge to form still larger lymphatic trunks (Figure 3).

[Figure 3 – Structure of a typical lymphatic capillary. Notice that interstitial fluid from the Interstitium compartments enters through clefts between overlapping endothelial cells that form the wall of the vessel. Valves ensure one-way flow of the interstitial fluid now called lymphatic fluid out of the tissue. Small collagen fibers of the Interstitium anchor the wall of the lymphatic capillary to the surrounding and cells, thus holding it open to allow entry of fluids and small particles.[13]
Lymphatic Trunks and Ducts
Lymphatic trunks drain lymphatic fluid from large regions in the body. The lymphatic trunks are usually named after the region they serve, such as the subclavian trunk that drains the arm. There are many lymphatic trunks throughout the body. These lymphatic trunks then join one of two collecting ducts, the thoracic duct or the right lymphatic duct (Figure 4)
Lymphatic trunks from the upper half of the right side of the body converge to form the right lymphatic duct, which empties into the right subclavian vein. Drainage from the remainder of the body is by way of the thoracic duct, which empties into the left subclavian vein.

]Figure 4 – Lymphatic drainage. The right lymphatic duct drains lymph from the upper right quadrant (dark blue) of the body into the right subclavian vein. The thoracic duct drains lymph from the rest of the body (green) into the left subclavian vein. The lymphatic fluid is thus returned to the systemic blood just before entering the heart.][13]
Lymphatic or Lymph Nodes
Lymph nodes, which are frequently called glands but are not true glands, are small bean=shaped bodies of lymphatic tissue found in groups of two to fifteen along the course of the lymphatic vessels (Figure 5). Major locations of lymph nodes are in the following regions: cervical, axillary, inguinal, pelvic cavity, abdominal cavity, and thoracic cavity. Lymph nodes vary in size and act as filters to remove bacterial phages or cellular particles from the lymphatic fluid stream. Lymph nodes contain white blood cells called lymphocytes, which release alkaline compounds such as SO-, OH- and hydrogen peroxide or H2O2 to buffer acidic metabolic wastes from the interstitial fluids of the Interstitium. Lymph nodes also contain white blood cells call macrophages, which pick up bacterial pHages or cell fragments, damaged cells, and cellular debris called endotoxins. [13][14]

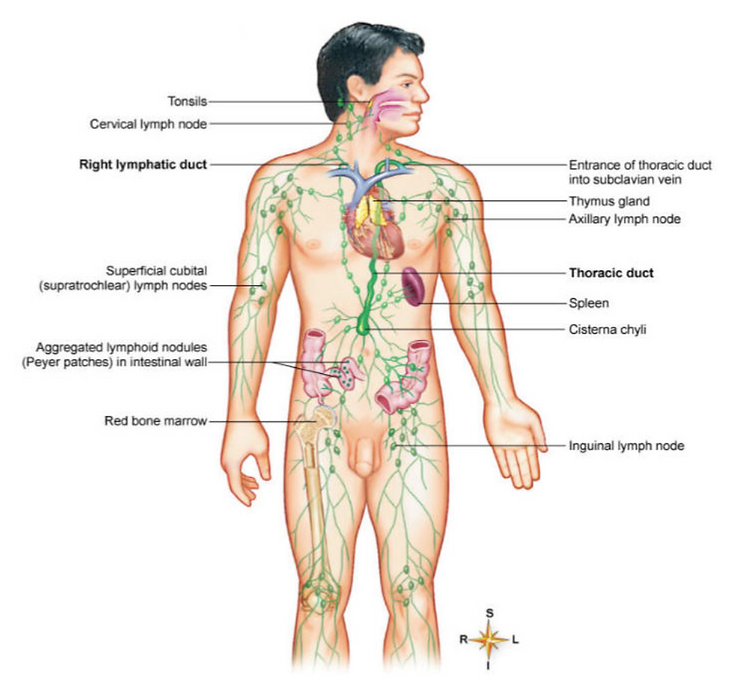
[Figure 5 – Principal organs of the lymphatic system.][13]
References
[1] Rodney A. Rhoades; David R. Bell (18 January 2012). Medical Phisiology: Principles for Clinical Medicine. Lippincott Williams & Wilkins. pp. 5–6. ISBN 978-1-60913-427-3.
[2] Jacob M, Chappell D, Rehm M (2009). “The ‘third space’–fact or fiction?”. Best Pract Res Clin Anaesthesiol. 23 (2): 145–57. PMID 19653435.
[3] Brown, Thomas A. (2011). Rapid Review Physiology. Elsevier Health Sciences. p. 2. ISBN 0323072607.
[4[ Abid.
[5] Barbara Kuhn Timby (1 January 2008). Fundamental Nursing Skills and Concepts. Lippincott Williams & Wilkins. pp. 319–. ISBN 978-0-7817-7909-8. Retrieved 9 June 2010.
[6] Redden M, Wotton K (June 2002). “Third-space fluid shift in elderly patients undergoing gastrointestinal surgery: Part 1: Pathophysiological mechanisms”. Contemp Nurse. 12 (3): 275–83. PMID 12219956.
[7] Drain, Cecil B. (2003). Perianesthesia nursing: a critical care approach. Philadelphia: W.B. Saunders Co. ISBN 0-7216-9257-5.
[8] “FLUID AND ELECTROLYTE THERAPY”. Archived from the original on 2010-07-07. Retrieved 2010-06-08.
[9] Mass spectrometry in cancer biomarker research: A case for immunodepletion of abundant blood-derived proteins from clinical tissue specimens – Scientific Figure on ResearchGate. Available from: https://www.researchgate.net/figure/Distribution-of-blood-lymph-and-interstitial-fluid-in-human-tissue-Tissue-embedded_fig2_260167519 [accessed 25 Jan, 2020]
[10] www.encyclopedia.lubopitko-bg.com Corporation. Capillary Exchange. http://Biomark Med. Author manuscript; available in PMC 2014 December 01.
[11] “Systematic Review of Hypotonic Versus Isotonic Intravenous Fluids”. 2013.
[12] Feld, LG; Neuspiel, DR; Foster, BA; Leu, MG; Garber, MD; Austin, K; Basu, RK; Conway EE, Jr; Fehr, JJ; Hawkins, C; Kaplan, RL; Rowe, EV; Waseem, M; Moritz, ML; SUBCOMMITTEE ON FLUID AND ELECTROLYTE, THERAPY. (December 2018). “Clinical Practice Guideline: Maintenance Intravenous Fluids in Children”. Pediatrics. 142(6): e20183083. doi:10.1542/peds.2018-3083. PMID 30478247.
[13] Thibedeau, G. A., & Patton, K. T. (2006). Anatomy & Physiology (6th ed.). St. Louis: Elsevier Health Sciences
[14] www.drrobertyoung.com